Menstrual Migraines: The Hormone Connection That Can Help Prevent Them
Why are women three times more likely to get migraines than men?
Hormones.
The rise and fall of estrogen throughout the menstrual cycle can trigger migraines. Most women who experience this just push through. They've tried the usual treatments, but nothing really helps because they're treating the pain, not the cause.
Menstrual migraines are harder to treat. They last longer, hurt more, and linger for days. But when hormones are the trigger, hormones can also be part of the prevention.
So What's Actually Happening? What Is a Menstrual Migraine or Headache?
Whether it's a full-blown migraine or a persistent headache, the mechanism is the same: it's linked to hormone changes in the menstrual cycle. Specifically, the drop in estrogen. It's not about having too much or too little. It's about the rapid change. The classic timing is anywhere from 2 to 5 days before your period starts (when estrogen drops to trigger menstruation) to about 3 days after bleeding begins (when estrogen starts to rise back up).
During the hormone changes, your brain becomes more sensitive to pain. On top of that, other known migraine triggers are happening at the same time: serotonin levels drop, inflammation increases, and iron and magnesium levels fall. It's a perfect storm. And it's why women with menstrual migraines often experience cramps, mood changes, PMS, or PMDD. They're all connected.
There are two types of migraines related to your cycle:
Pure menstrual migraine: You only get migraines around your period and at no other time. This is less common (about 10-15% of women with menstrual migraines).
Menstrually related migraine: You get migraines around your period, but also at other times during the month. This is more common. And even when treatment reduces your overall migraine frequency, the menstrual ones often stick around. They're stubborn.
Knowing which type you have helps determine the best treatment and management approach. And the only way to figure that out? Tracking.
Why Tracking Matters
Keep a migraine diary for 2-3 cycles. Track when migraines start and end, severity, and where you are in your cycle. We can only confirm a migraine was "menstrual" in hindsight, once your period arrives.
What if you don't have a period?
Women using hormonal IUDs, those who've had ablation, or anyone with a partial hysterectomy might not bleed but may still be cycling hormonally. Tracking symptoms like breast tenderness, bloating, or mood changes can help. If those symptoms correlate with your headaches, or if your migraines seem to happen on a predictable frequency, there's likely a hormonal connection.
What Changes in Perimenopause
If you're in your late 30s or 40s and your migraines are suddenly worse, more frequent, or have returned after years of being migraine-free, perimenopause might be the culprit.
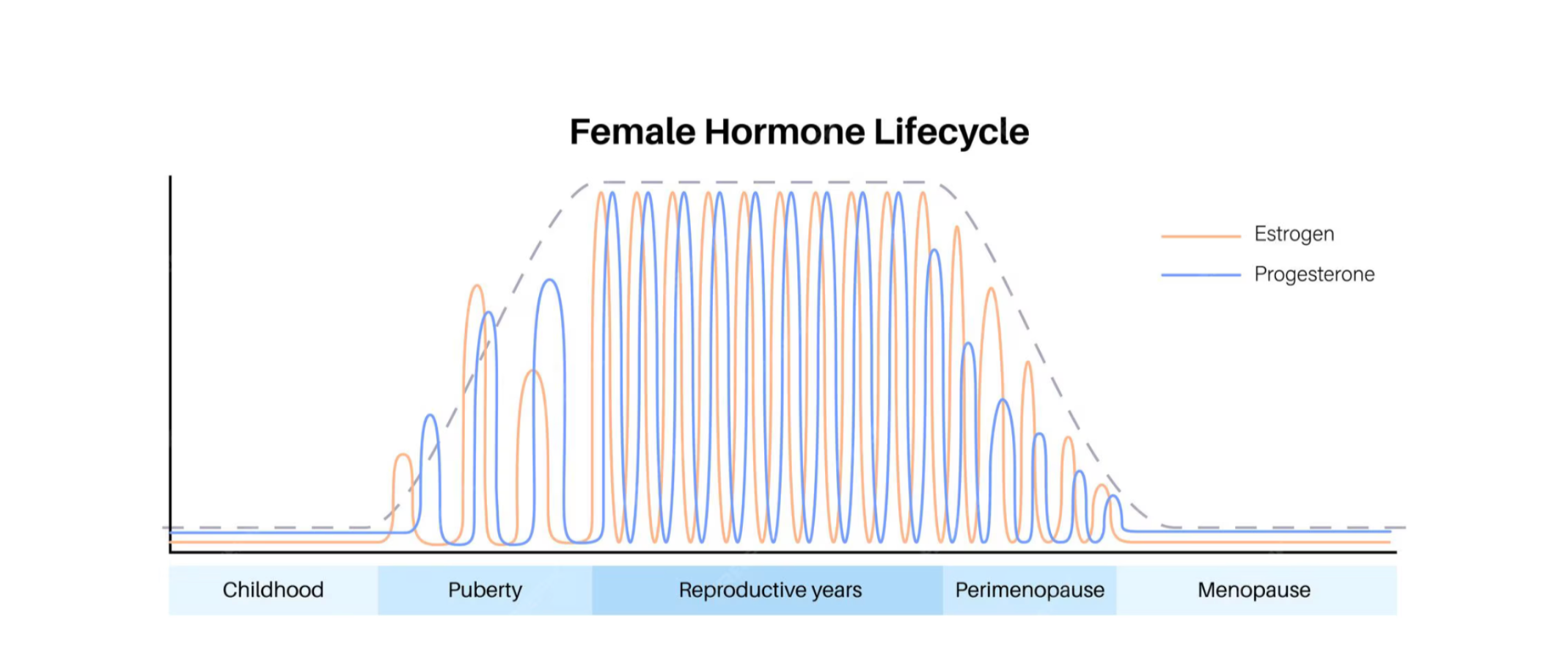
During perimenopause, estrogen doesn't decline gradually. It fluctuates wildly. One month higher than your 20s, the next much lower. These unpredictable swings create more frequent, more dramatic estrogen drops, which means more migraine triggers.
Many women I see had migraines during puberty (another time of hormonal chaos), then they settled down, and now they're back with a vengeance in perimenopause. Sound familiar?
The good news? Once through menopause, many women find their migraines improve as hormones stabilize. But you don't have to white-knuckle it through perimenopause waiting for that.
Using Estrogen to Soften the Drop
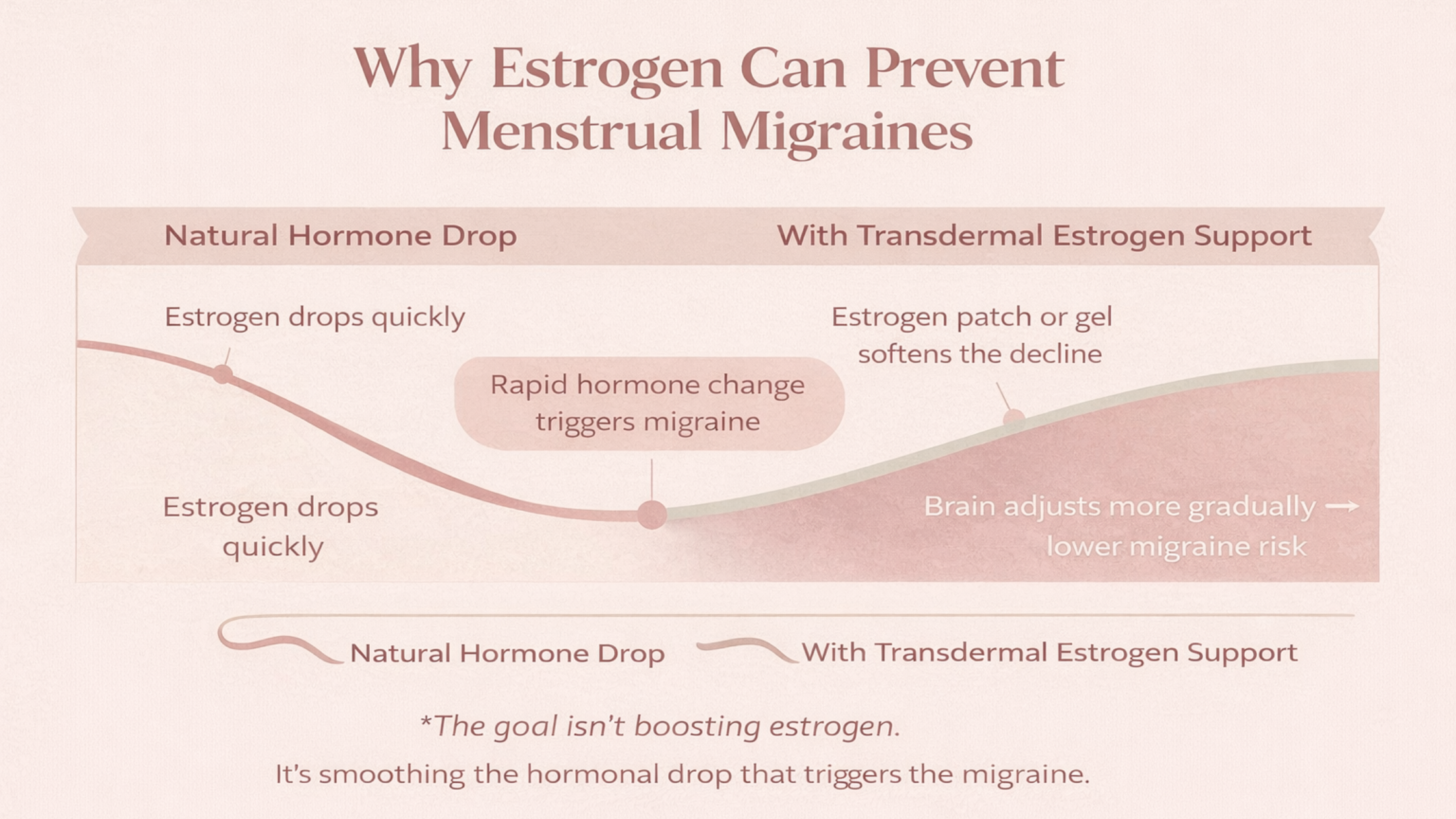
Here's what most people don't understand about using estrogen for menstrual migraines: the goal isn't to "boost" your estrogen. It's to smooth out the drop.
Transdermal estrogen (a patch or gel) used around your period creates a more gradual decline instead of a steep cliff. This gentler change gives your brain time to adjust without triggering a migraine.
Timing matters. Your goal would be to start the estrogen before the migraine usually happens, and continue for the first few days of your cycle. This is where tracking becomes essential.
A quick side note: What about progesterone?
You've likely heard that if you're taking estrogen and have a uterus, you need progesterone too. And you're right. But for short-term, cyclical use like this (just a few days around your period), your body is still producing its own progesterone, which is doing that protective work. So we generally don't need to add it.
What if I have migraines with aura?
You may have been told you can't take estrogen at all. That's not quite right. Migraines with aura are a contraindication to oral estrogen (like birth control pills) due to stroke risk. But transdermal estrogen bypasses the liver entirely, so it doesn't carry the same clotting concerns. It will likely still be an option depending on your individual risk factors. It's a conversation worth having with a provider who understands the nuance.
Other Approaches
Estrogen therapy targets the hormone-related migraines specifically. But if you also experience migraines outside of that timeframe, these other approaches can help reduce your overall migraine burden. For many women, it's a combination of both.
Lifestyle factors that support hormonal stability: Consistent sleep, balanced meals to prevent blood sugar swings, stress management, regular movement, and limiting alcohol and nicotine.
Acupuncture has been shown to reduce the severity of menstrual migraines.
Supplements like magnesium, vitamin B2, and iron (when repletion is necessary) can support overall migraine prevention. These don't directly address the hormonal trigger, but they're part of the bigger picture.
The Bottom Line
Menstrual migraines aren't "bad luck" or something you have to accept. They're tied to predictable hormonal shifts, and once we understand your pattern, there are real options for prevention.
Whether you're 28 and have dealt with this since your teens, or you're 45 wondering why your migraines are suddenly back, tracking your symptoms and exploring targeted treatment can change things.
You don't have to keep canceling plans, pushing through workdays in pain, or dreading the same week every month.
If this sounds like you (or someone you know), our team at Ivy would love to help. Reach out to book a meet-and-greet and let's talk about what's possible.
Frequently Asked Questions:
-
Track your migraines alongside your cycle for 2-3 months. If at least two-thirds occur in those few days around your period, there's likely a hormonal connection.
-
Absolutely. The hormonal instability of perimenopause can trigger migraines in women who never experienced them during their regular cycling years. It's one of the lesser-known symptoms of this transition.
-
The goal is to prevent the rapid estrogen drop that triggers the migraine. Transdermal estrogen (a patch or gel) creates a gentler decline instead of a steep cliff. You start it before your typical migraine timing and continue through the first few days of your cycle. It's prevention, not rescue.
A note on language: While this article uses "women" for readability, menstrual migraines can affect anyone who menstruates, regardless of gender identity.